Quick answer: QOF 2026/27 introduces six new or significantly changed indicators that Practice Managers must prepare for now. DM037 requires all 8 NICE diabetes care processes per patient, HF009 mandates 4-pillar heart failure therapy, OB004 and OB005 replace the Weight Management Enhanced Service with 18 new obesity points, and CD001/CD002 consolidate cardiovascular blood pressure control with a new frailty coding dependency. Vaccination indicators (VI001, VI002, VI003) now include the MMRV vaccine and offer improvement thresholds that reward gains from each practice’s own baseline.
If you are a Practice Manager, QOF Lead, or GP Partner looking for a clear, actionable summary of what is changing in the 2026/27 Quality and Outcomes Framework, this guide walks you through every new indicator, the point values at stake, and the exact register audits you should be running this week.
What is changing in QOF 2026/27?
The QOF 2026/27 framework introduces six new or significantly restructured indicators alongside point reallocations across the existing framework. The headline changes are:
- DM037 replaces DM012 and demands all 8 NICE diabetes care processes annually
- HF009 replaces HF003 and HF006, requiring 4-pillar heart failure therapy for HFrEF patients
- OB004 and OB005 are brand new obesity indicators worth 18 points combined
- CD001 and CD002 consolidate four older indicators (CHD015, CHD016, STIA014, STIA015) into a single blood pressure framework with frailty exclusions
- VI001, VI002, VI003 add the MMRV vaccine and introduce improvement thresholds
- CHOL003 drops from 38 to 20 points, while DM034 and DM035 statin indicators both rise to 8 points each
The total QOF point value for 2026/27 is £227.95, a 1.1% increase from the previous year, although list size adjustments mean the cash value per practice is broadly unchanged.
QOF 2026/27 new indicators at a glance
| Indicator | What it measures | Thresholds | Points | Replaces |
|---|---|---|---|---|
| DM037 | All 8 NICE diabetes care processes delivered annually | 40 to 90% | 10 | DM012 |
| HF009 | 4-pillar therapy in heart failure with reduced ejection fraction | 20 to 50% | 12 | HF003, HF006 |
| OB004 | Referral to weight management for adults with obesity | 10 to 30% | 5 | Weight Management Enhanced Service |
| OB005 | Shared decision-making and pharmacotherapy for obesity | 50 to 80% | 13 | Weight Management Enhanced Service |
| CD001 | Blood pressure control, age 79 or under, no frailty | 40 to 90% | 41 | CHD015, CHD016, STIA014, STIA015 |
| CD002 | Blood pressure control, age 79 or under, no frailty (second threshold) | 46 to 90% | 20 | As above |
DM037 explained: the 8 diabetes care processes
DM037 is the indicator most likely to catch unprepared practices out. It requires delivery of all 8 NICE-recommended care processes for patients with Type 2 diabetes, drawn from NICE guideline NG28 and tracked by the National Diabetes Audit.
The 8 NICE diabetes care processes
- HbA1c measurement
- Blood pressure measurement
- Serum cholesterol measurement
- Serum creatinine and eGFR
- Urine albumin-to-creatinine ratio (ACR)
- Foot examination
- BMI or weight measurement
- Smoking status recording
This is an all-or-nothing indicator. A patient who receives 7 out of 8 care processes does not count toward your numerator. Only patients completing the full set contribute.
National Diabetes Audit data shows that only around 50 to 55% of Type 2 diabetes patients currently receive all 8 processes. The most commonly missed are urine ACR testing and foot examination, both of which require dedicated appointment actions rather than a single blood draw.
Note that retinal screening is the ninth process tracked by the National Diabetes Audit but is delivered by the national screening programme, not by GP practices. It is not included in DM037.
What Practice Managers should do now for DM037
- Run a search for all diabetic patients missing any of the 8 processes in the last 12 months
- Identify the specific gaps, with urine ACR and foot checks typically the largest
- Ensure your annual diabetes review template captures all 8 processes with extractable SNOMED codes
- Build recall workflows that batch patients by missing process, not by appointment type
HF009 explained: the 4 pillars of heart failure therapy
NICE indicator specification IND317, published in November 2025, maps directly to HF009. The indicator covers patients with heart failure and reduced ejection fraction (HFrEF, defined as left ventricular ejection fraction of 40% or less).
The 4 pillars of HFrEF treatment
- ACE inhibitor, ARB, or ARNI (sacubitril-valsartan)
- Beta-blocker licensed for heart failure (bisoprolol, carvedilol, or nebivolol)
- Mineralocorticoid receptor antagonist (spironolactone or eplerenone)
- SGLT2 inhibitor (dapagliflozin or empagliflozin)
National data suggests only around 15% of HFrEF patients are currently on all four pillars, which is why the upper threshold has been set at a deliberately achievable 50%. The most commonly missing pillar is the SGLT2 inhibitor, since many patients were stabilised on three drugs before SGLT2 inhibitors entered NICE guidance.
What Practice Managers should do now for HF009
- Search the heart failure register for patients coded with HFrEF specifically
- For each patient, audit how many pillars they are currently prescribed
- Identify patients on 2 or 3 pillars who could be optimised with the addition of a missing class
- Assign the work to your clinical pharmacist or PCN pharmacist as a lead role
- Document any contraindications or intolerances clearly so exception reporting is available
OB004 and OB005 explained: the new obesity indicators
OB004 and OB005 mark the return of obesity to QOF after a one-year gap, replacing the retired Weight Management Enhanced Service. Together they are worth 18 points.
OB004: referral to weight management
OB004 is worth 5 points with thresholds of 10 to 30%. It requires that eligible adults with obesity are offered a referral to a structured weight management programme (Tier 2 community lifestyle services or Tier 3 specialist multidisciplinary services) within 90 days of the BMI being recorded.
NICE guideline NG246 sets the referral criteria, including ethnicity-adjusted BMI thresholds:
- BMI of 30 or above for most adults
- BMI of 27.5 or above for people of South Asian, Chinese, other Asian, Middle Eastern, Black African, or African-Caribbean family background
OB005: shared decision-making and pharmacotherapy
OB005 is worth 13 points with thresholds of 50 to 80%. It covers shared decision-making conversations and pharmacotherapy for obesity, including NICE-approved medications such as orlistat, liraglutide (Saxenda), semaglutide (Wegovy), and tirzepatide (Mounjaro).
A key open question for Practice Managers is whether OB005 requires an actual prescription or whether a documented shared decision-making conversation (including a mutual decision not to prescribe) is sufficient. The business rules will clarify this, but the achievability gap between those two interpretations is significant.
What Practice Managers should do now for OB004 and OB005
- Identify your obesity register using both standard and ethnicity-adjusted BMI thresholds
- Map local Tier 2 and Tier 3 weight management referral pathways
- Audit current obesity pharmacotherapy prescribing to identify eligible but untreated patients
- Build a shared decision-making consultation template that records decisions in extractable form
- Compare your 2025/26 Weight Management Enhanced Service income with realistic OB004/OB005 projections
CD001 and CD002 explained: consolidated blood pressure control
CD001 (41 points) and CD002 (20 points) replace four older indicators (CHD015, CHD016, STIA014, STIA015), consolidating cardiovascular blood pressure control into a simpler structure. Both apply to patients aged 79 or under without moderate or severe frailty.
Why frailty coding now matters more than ever
The exact frailty definition is expected to align with the Electronic Frailty Index (eFI):
- Fit: eFI 0 to 0.12
- Mild frailty: 0.13 to 0.24
- Moderate frailty: 0.25 to 0.36
- Severe frailty: above 0.36
Patients with moderate or severe frailty will be excluded from CD001 and CD002, which means poor frailty coding will lose you points in two ways: it includes patients who should be excluded, and it pushes your overall achievement rate down.
What Practice Managers should do now for CD001 and CD002
- Run your eFI calculation if your clinical system supports it
- Audit how many patients on your cardiovascular registers have frailty status coded
- Prioritise frailty coding for patients aged 65 and over on CVD registers
- Brief clinicians that frailty coding is now a QOF income driver, not just a clinical record
Vaccination improvement thresholds: a new mechanism for low-uptake areas
The childhood vaccination indicators (VI001, VI002, VI003) now include the MMRV vaccine (measles, mumps, rubella, varicella) and introduce a second route to points based on improvement from your own 2-year baseline.
From 2026/27, practices earn points through whichever route is higher:
- The traditional achievement thresholds (89 to 96%, 86 to 96%, 81 to 96%), or
- A sliding scale starting 5 percentage points above your practice’s 2-year average
For VI001, the improvement upper threshold is 18 percentage points above baseline. For VI002 it is 23 percentage points. For VI003 it is 30 percentage points.
This is particularly valuable for practices in London and other areas with historically low uptake, where the standard thresholds have been effectively unreachable.
What Practice Managers should do now for vaccinations
- Pull your 2-year vaccination averages for VI001, VI002, and VI003
- Calculate your improvement thresholds
- If the improvement route offers a realistic path that the standard route does not, build a targeted vaccination improvement plan
Other QOF 2026/27 changes Practice Managers need to model
Beyond the new indicators, several existing indicators have changed point allocations:
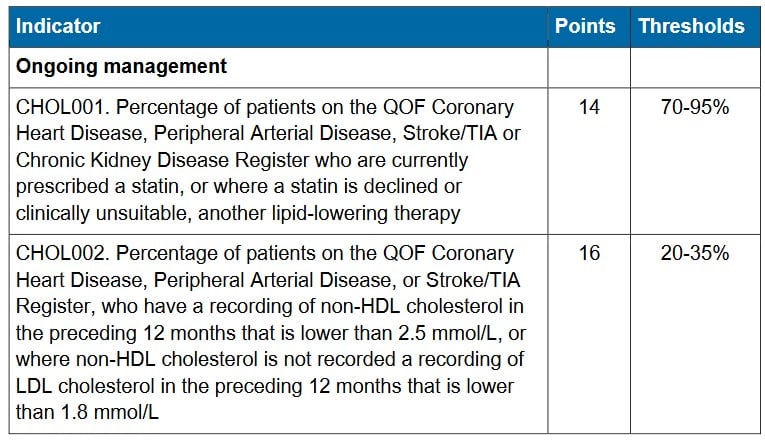
- CHOL003 drops from 38 to 20 points — a meaningful income reduction for practices that were achieving well
- DM034 (primary prevention statin use) rises from 4 to 8 points
- DM035 (secondary prevention statin use) rises from 2 to 8 points
- NDH003 rises from 18 to 20 points and now includes women with previous gestational diabetes
- AF006 upper threshold increases from 90% to 95%
- STIA007 adds ticagrelor to the antiplatelet medication list
- Asthma register now includes patients from age 5
- COPD register business rules are updated to address under and over-recording identified by audit
QOF 2026/27 preparation checklist for Practice Managers
| When | Action |
|---|---|
| This week | Run register audits: diabetes (8 processes), heart failure (4 pillars), obesity (BMI register), frailty coding |
| This week | Identify gaps in diabetes care processes, focusing on urine ACR and foot examination |
| This month | Review HFrEF patients for 4-pillar optimisation with your clinical pharmacist |
| This month | Map local weight management referral pathways (Tier 2 and Tier 3) |
| This month | Calculate vaccination 2-year baselines for VI001, VI002, VI003 |
| This month | Model CHOL003 point reduction impact on your practice income |
| Ongoing | Update clinical system templates when your supplier releases the QOF v51 update |
| From April | Begin coding to the new indicators from day one of the contract year |
Frequently asked questions about QOF 2026/27
When does QOF 2026/27 start?
QOF 2026/27 runs from 1 April 2026 to 31 March 2027. Coding against the new indicators should begin from the first day of the contract year.
What is the value of a QOF point in 2026/27?
The value of a QOF point in 2026/27 is £227.95, a 1.1% increase on the previous year. The Contractor Population Index is used to weight this against your registered list size.
How many new QOF indicators are there in 2026/27?
There are six new or significantly restructured QOF indicators in 2026/27: DM037, HF009, OB004, OB005, CD001, and CD002. The three childhood vaccination indicators (VI001, VI002, VI003) have also been updated with MMRV inclusion and improvement thresholds.
What is DM037 in QOF?
DM037 is a new diabetes indicator worth 10 points that requires delivery of all 8 NICE-recommended diabetes care processes (HbA1c, blood pressure, cholesterol, eGFR, urine ACR, foot examination, BMI, and smoking status) to each Type 2 diabetes patient within the QOF year. It is an all-or-nothing indicator.
What does HF009 require?
HF009 requires patients with heart failure and reduced ejection fraction (HFrEF) to be prescribed all 4 pillars of disease-modifying therapy: an ACE inhibitor, ARB or ARNI; a heart failure beta-blocker; a mineralocorticoid receptor antagonist; and an SGLT2 inhibitor. It is worth 12 points with thresholds of 20 to 50%.
Are OB004 and OB005 replacing the Weight Management Enhanced Service?
Yes. The Weight Management Enhanced Service is retired in 2026/27. OB004 (5 points) covers referral to structured weight management, and OB005 (13 points) covers shared decision-making and pharmacotherapy. Whether your practice is financially better or worse off depends on your historical referral volume.
How do the new vaccination improvement thresholds work?
VI001, VI002, and VI003 now offer two routes to points: the traditional achievement thresholds, or a new improvement route that starts 5 percentage points above your practice’s 2-year baseline uptake. Practices receive whichever allocation is higher at year-end.
The bottom line for Practice Managers
The clinical definitions behind every new QOF 2026/27 indicator are already published in NICE guidance. Practices that wait for the v51 business rules and clinical system template updates before starting their register audits will lose 6 weeks of preparation time. The Practice Managers who win in 2026/27 will be those who treat QOF preparation as a year-round data quality and recall planning exercise, not an April rush.
Start with the four register audits listed in the checklist above. Brief your clinical team on the four highest-stakes changes (DM037, HF009, the obesity indicators, and frailty coding for CD001/CD002). Model your projected income against the point reallocations. The work is the same whether the business rules drop tomorrow or in March.
Primary NHS England sources
NHS England — Changes to the GP Contract in 2026/27 (24 February 2026 letter)
NHS England — 2026/27 QOF guidance
NHS England — Statement of Financial Entitlements Directions
NICE clinical guidance
NICE NG28 — Type 2 diabetes in adults: management
NICE NG106 — Chronic heart failure in adults: diagnosis and management
NICE IND317 — Heart failure 4-pillar therapy indicator specification
NICE NG246 — Overweight and obesity management
NICE TA875 — Semaglutide (Wegovy) for managing overweight and obesity
NICE TA1026 — Tirzepatide for managing overweight and obesity
NICE TA664 — Liraglutide (Saxenda) for managing overweight and obesity
NICE TA235 — Orlistat for the treatment of obesity
Audit and data sources
National Diabetes Audit (NHS England)
Electronic Frailty Index (eFI) — Clegg et al., Age and Ageing 2016
Secondary commentary
Queen Mary University of London CEG — QOF 2026/27 changes: what we know so far (PDF)
Management in Practice — Making the most of QOF 2026/27, by Dr Gavin Jamie
Practice Index — A practical view of the QOF 26/27 changes, by Ceri Gardener
Practice Index — 2025/26 QOF summary
Londonwide LMCs — Initial response and analysis: GMS Contract changes 2026/27
Insight Solutions — QOF 2026/27 summary
This article is for informational purposes only and reflects QOF 2026/27 guidance as published. Practices should refer to the latest official NHS England contract documents and v51 QOF business rules when these are released.